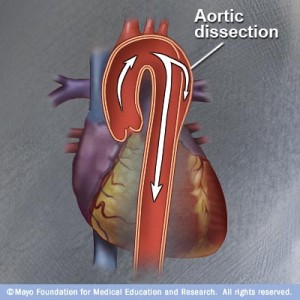
 Aortic dissection is a condition of the major artery that pumps blood from the heart. When a tear develops in the inner layer of the vessel, blood leaks at high volumes through this tear into the middle layer of the aorta. The layers begin to separate and bulge (dissect). If the blood-filled channel ruptures through the outside aortic wall, the dissection is often fatal. Symptoms of an aortic dissection include severe chest pain radiating to the back, nausea, shortness of breath, and sweating.
Aortic dissection is a condition of the major artery that pumps blood from the heart. When a tear develops in the inner layer of the vessel, blood leaks at high volumes through this tear into the middle layer of the aorta. The layers begin to separate and bulge (dissect). If the blood-filled channel ruptures through the outside aortic wall, the dissection is often fatal. Symptoms of an aortic dissection include severe chest pain radiating to the back, nausea, shortness of breath, and sweating.
On the night of May 12, 2008, Ms. A was seen in the emergency room of McKenzie Memorial Hospital in Sandusky, Michigan, for severe chest pain that she rated at a level nine out of ten. The pain, which she described as burning and pressure, radiated through her back. She felt nauseated, and complained that she was short of breath.
Dr. K, an obstetrician/gynecologist who was moonlighting in the emergency room that night, evaluated Ms. A. A chest x-ray revealed a widened mediastinum (part of the chest cavity containing the heart and lungs), which is an indication that an aortic dissection could exist. Dr. K consulted another physician, Dr. E, an internal medicine specialist. The physicians decided to give her blood thinners and transfer her to Covenant Medical Center in Saginaw, Michigan, where they believed she could receive the level of care she required.
While in the emergency room of Covenant, Ms. A was seen by Dr. M who diagnosed her with unstable angina, a type of chest pain caused by reduced blood flow to the heart. Ms. A was admitted to the hospital’s telemetry unit at 4 a.m. on May 13, for continuous monitoring of her heart. Nurses were told that there was no need to call Dr. D, the cardiologist who Ms. A was admitted under, until after 7 a.m. Ms. S still did not receive critical diagnostic tests that would have indicated that she had an aortic dissection.
Just after 5 a.m., the nurse taking care of Ms. A noted that she was very nauseated and started to vomit. Ms. A’s vital signs were abnormal and she was visibly pale. Yet, the nurse failed to call Dr. D for instructions.
The nurse discovered Ms. A just after 6 a.m. in full cardiac arrest. Hospital staff attempted to resuscitate Ms. A by inserting a breathing tube, administering emergency medications, and restoring regular heart rhythms (defibrillation). None of these measures were successful. Ms. A passed away at 6:35 a.m. The autopsy report revealed that Ms. A died as a result of a large amount of blood that had collected in her chest, preventing her heart from pumping properly. The blood came from a tear that formed in her aorta that went negligently undiagnosed by the physicians and nurses at both McKenzie and Covenant.
Jules Olsman will represent the family of Ms. A in a case against the physicians, nurses, and hospitals who failed to recognize the signs and symptoms of her aortic dissection and provide timely treatment which would have saved her life.
Source: //www.mayoclinic.com/health/aortic-dissection/DS00605